By Lance Chilton
Back about a millennium ago – or so it seems – New Yorkers, Frenchmen, residents of Indian cities and Vancouverites would gather on their apartments’ balconies banging pots at a defined hour as a tribute to health care workers’ actions during the pandemic. Just a few weeks ago, a massive march honoring essential workers was held in New York City, but in much of the US, the sacrifices made by health care workers seem to have gone under the radar.
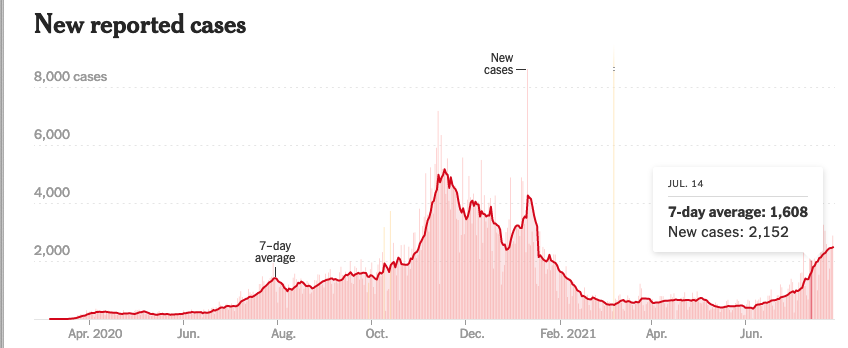
That doesn’t mean that those sacrifices are over, just as the pandemic is clearly not over, showing signs of a fourth wave in every state in the United States and most countries throughout the world. Health care workers routinely care for people with COVID, some who know it, some who don’t – in outpatient clinics, emergency rooms, hospital wards, and intensive care units. Contagion doesn’t respect status: clerks, aides, nurses and doctors have all been infected and are among the 610,000+ Americans who have died of this unique disease.
The New York Times on July 1, 2021 published an article entitled “Frontline Health Care Workers Aren’t Feeling the ‘Summer of Joy’”. The article quotes a Missouri critical care specialist as saying of his colleagues, “They’re weary and they’re also disappointed that the country has started the end zone dance before we cross the goal line. The truth is we’re fumbling the ball before we even get there.”
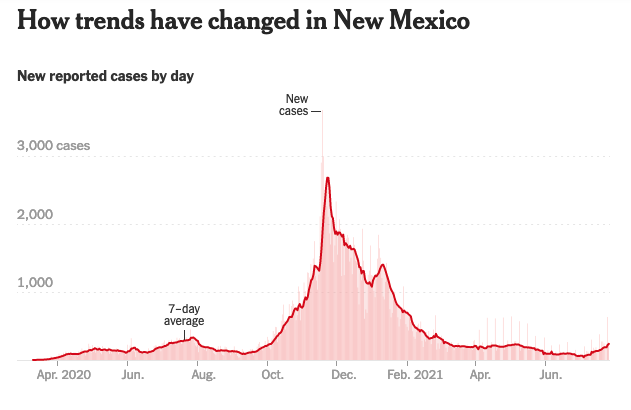
Missouri, of course, lacks the kind of coordinated, science-based response to the pandemic shown by our governor and her advisors; adult Missourians are 41% fully vaccinated, compared with New Mexico’s 57%. So problems aren’t quite as bad here, though fatigue and burnout are common among New Mexico’s frontline health care workers as well, and daily COVID case counts are increasing here too.
I spoke with a young nurse caring for day surgery patients in an Albuquerque medical center about her experiences with COVID. She said that at the onset of the pandemic, she had been working in one of our city’s hospitals’ acute care wards. “We had new COVID patients flown in almost every day; they would replace those who had died overnight. It was too much to bear. I had to get out to something less stressful!”
During much of the pandemic, hospitalized patients could not receive visitors, so nurses and other care personnel had to serve not only the medical needs of their critically ill patients, but also their emotional needs. They worked long hours and had to worry not only about their patients, but also about their families. What if they slipped up with their Personal Protective Equipment and got infected? Would they be taking the virus home?
My nurse informant told me of the Heroes Research Project (heroesresearch.org) where over 25,000 health care providers have signed up to record their reactions as they make their way through long days with COVID patients. Duke University medical researcher Emily O’Brien Ph.D. leads the federally-funded study. In an article published July 2 in the CDC journal MMWR, its authors indicated that “Among 26,174 respondents, 53.0% reported symptoms of at least one mental health condition in the preceding 2 weeks, including depression (32.0%), anxiety (30.3%), PTSD (36.8%), or suicidal ideation (8.4%).”
Burnout symptoms among medical care personnel were common before the pandemic – they work long hours in often difficult conditions. Some stick it out, some leave more stressful parts of the profession for less stressful parts; some leave the profession entirely. New Mexico can’t afford to lose health care providers – we’re already at a deficit, with 32 of New Mexico’s 33 counties being all or part officially-designated health care shortage areas. This is made even more worrisome, considering that New Mexico has the oldest physician workforce in the country, and many will leave practice before long. Nurses, too, are in short supply — Dr. Christine Kasper, dean of UNM College of Nursing, estimated at the end of last year that New Mexico has need for some 6000 more of these all-important health practitioners.
What can we do about COVID-induced burnout among health care professionals? How can we train enough new ones when COVID-induced fear and anxiety and lack of appreciation drive potential practitioners away from these professions? Bang pots, for sure, and realize that your providers need your concern and support too. And also support policies such as those passed by our Legislature in recent years and signed by Governor Luján Grisham, to increase supply. I’ll write more about those in an upcoming column.